Left Ventricle Angiography
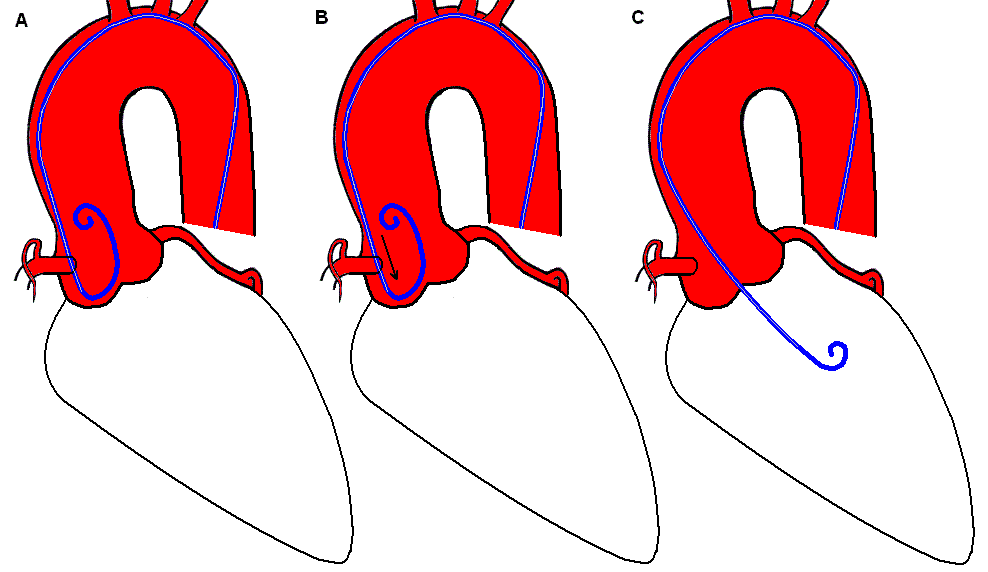
The pigtail catheter is used for LV angiography due to its ability to deliver large volumes of contrast with its end- and multiple side holes. The pigtail catheter can cross the valve directly with normal aortic valves. In many cases, it may be necessary to advance the pigtail down into one of the sinuses of Valsalva to form a secondary loop like the figure 6 A. As the catheter is withdrawn slowly B, this loop will open to span the full diameter of the aorta, at which point a very subtle further withdrawal will often cause the pigtail to fall across the valve C.
A 0.038-inch straight guidewire can aid the crossing of valve when aortic stenosis is present. With the wire tip positioned so that it is directed toward the aortic orifice, the tip of the wire usually quivers in the systolic jet. Wire and catheter are then advanced as a unit until the wire crosses into the left ventricle. If crossing is unsuccessful with straight wire and pigtail catheter, try using a left amplatz (AL1) catheter. In either case, the wire should be withdrawn and cleaned and the catheter should be flushed every 3 minutes to avoid blood from clotting onto the wire and potentially embolizing. If the AL1 catheter is successful in crossing the aortic valve, It will be necessary to use an exchange wire to exchange the AL1 catheter with the pigtail catheter.
Once the pigtail catheter is in the left ventricle, avoid contact with the papillary muscles or positioning too close to the mitral valve to avoid producing artificial mitral regurgitation. A midcavity position is optimal for contrast injection.
A powered injector is used for the LV angiogram. A contrast bolus of 30 - 45 mL is delivered at a rate of 10 - 15 mL/sec. Setting a rate of rise at 0.5 seconds allows for smoother contrast delivery. Inform the patient that a warm sensation from contrast vasodilation will last for 30 to 60 seconds. During the injection, the operator should maintain handle of the catheter and sheath while observing both physiologic and fluoroscopic monitors for adverse events. Standard angiographic view of the Left ventricle is 30 degree RAO that allows visualization of the high lateral, anterior, apical and inferior LV walls. A 45 degree LAO view best identifies the lateal and septal LV walls.
Complications
- Cardiac Arrhythmias - ventricular tachycardia related to stimulation from catheter and or contrast injection
- Intramyocardial "staining" - deposition of contrast material into myocardial tissue due to catheter position in the LV
- Embolism - injection of air or thrombus
- Contrast-related complications - vasodilation followed by nausea and vomiting related to high-osmolar contrast
Measuring Ejection Fraction
Ejection Fraction (EF) is the percentage of blood being pumped from the heart with each heart beat. A normal EF ranges from 55 - 70%. When heart muscle becomes damaged and the Left Ventricle is unable to squeeze as well as it used to, the EF is diminished. In the cardiac cath lab, the EF is measured using the images of the Left Ventriculogram. This is known as an angiographic measurement of EF. The fluoroscopic system is usually equiped with options to measure the EF.
The calculation for EF = ( STROKE VOLUME / END DIASTOLIC VOLUME ) X 100.
The calculation for STROKE VOLUME = END DIASTOLIC VOLUME (EDV) - END SYSTOLIC VOLUME (ESV)
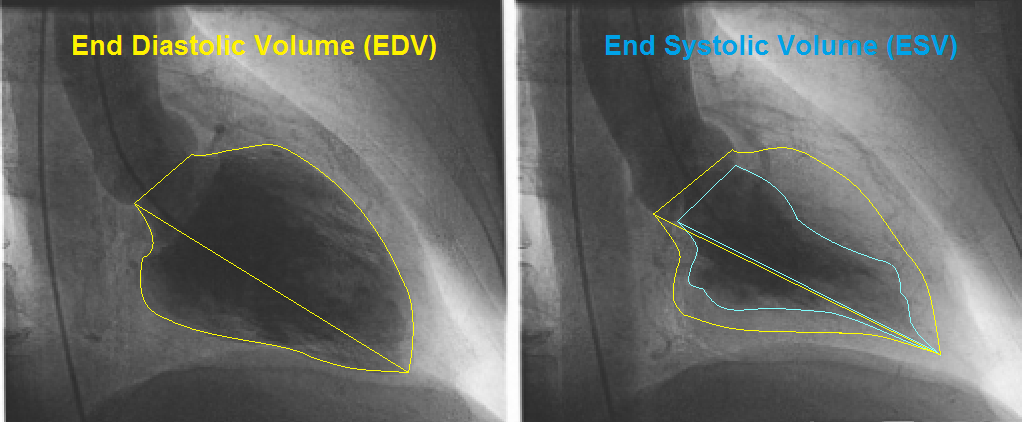
If the EDV is measured to be 144 mL and the ESV is measured to be 60 mL:
Stroke Volume = EDV - ESV
Stroke Volume = 144 mL - 60 mL
Stroke Volume = 84 mL.
EF = (SV / EDV) X 100
EF = (84 mL / 144 mL) x 100
EF = 58%.
References